Also abbreviated as KA, keratoacanthoma is the name of a type of skin malignancy which is identified by the occurrence of abnormal bumps on the skin. These bumps are shaped like a volcano and develop quite rapidly. The skin cancer is more prevalent in middle-aged adults and the elderly who have been exposed to the UV rays of the sun for prolonged periods of time. It is also possible for people belonging to all age groups to develop keratoacanthoma.
Scientists from all over the world consider a keratoacanthoma as a form of squamous cell carcinoma. However, a keratoacanthoma relatively much less aggressive in nature. Most cases of keratoacanthomas tend to cause minimal or restricted skin damage. Some patients may suffer from the extreme forms of keratoacanthoma; they may also be increasingly vulnerable to the spread of the cancer to the lymph node glands.
Symptoms
Some of the main signs and symptoms of keratoacanthoma skin cancer are as follows:
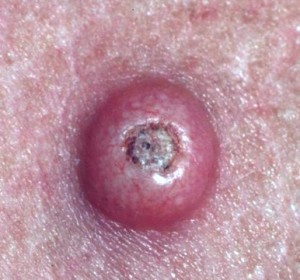
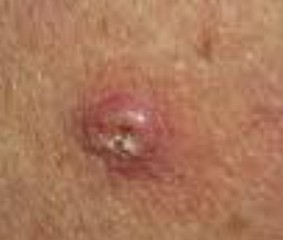
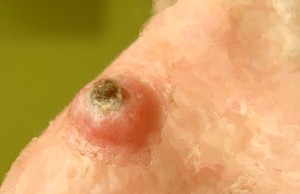
- In most cases, a keratoacanthoma will develop on the skin in the form of minor lesions. They often look like pimples. The skin abnormalities are made up of keratin which is one of the main substances occurring in nails, skin, and hair, etc.
- A majority of people suffering from the skin cancer tend to develop keratoacanthoma lesions on different parts of the body, but especially on the forearms, center region of the face, scalp, back portion of the hands, and on the ears. Occasionally, the bottom half of the lower limbs may also experience the occurrence of keratoacanthoma lesions; it is particularly prevalent in female patients.
- After the initial eruption of a keratoacanthoma lesion, it tends to grow at a brisk pace for about 2 to 7 weeks. Finally, it may turn into a dome-like bump with a minute dent in the center. Such a bump is usually flesh colored. The size of a fully grown keratoacanthoma bump tends to differ and ranges between 1 cm and 3 cm diametrically.
- A keratoacanthoma may not be accompanied by pain. However, some affected persons may experience itchiness and minor distress or discomfort. It may also be noted that, as per their location, the malignant lesions may hamper the normal functioning of the body part that they erupt on.
- It is also possible for keratoacanthomas to be an indicator of some other underlying ailment which is more dangerous than the skin cancer. This is however very rare.
Causes of keratoacanthoma
Keratoacanthoma skin cancer normally occurs in older adults who have fair skin as well as a history of exposure to UV rays for many decades.
Some of the risk factors which can increase the vulnerability to developing keratoacanthoma skin lesions are listed below:
- Excessive exposure to the rays of the sun or to other forms of UV light can pose elevated threat to keratoacanthoma skin cancer
- Individuals who are older than 50 years carry an additional risk as compared to younger people
- People featuring naturally light hair color, fairer skin, and eyes with light colors are more vulnerable than others.
- As compared to women, men are more susceptible to developing the malignant lesions
- Infection with the human papilla virus or HPV as well as with other specific strains belonging to the family of wart viruses increase the vulnerability.
- Use of immune system inhibiting medications for several weeks, months, or even years can increase the risk. People may take immunosuppressants to treat immune system disorders, or after an organ transplant, etc.
- Radiation therapy as treatment for previous cases of other types of cancers.
Other uncommon risk factors which can pose increased threat to development of keratoacanthoma malignancies include contact with tar and other kinds of toxic chemicals; ulcers which persist for long periods of time; an existing skin cancer illness; and extensive scarring of the skin as is seen after suffering from gasoline burns.
Treatment
Most instances of keratoacanthoma lesions tend to abruptly clear out on its own without treatment in about 5 to 7 months. The only reminder of the skin cancer is a scar mark which develops on the keratoacanthoma location.
It may be however noted that keratoacanthoma lesions can cause significant damage to the top layers of the skin as well as injure the tissues that occur underneath the epidermis. Also, some uncommon types of keratoacanthoma can spread to the deeper parts of the skin as well as other regions such as the lymph nodes. Keratoacanthoma lesions are also quite ugly in appearance. This can result in varied psychological problems like embarrassment, stress, lowered self-value, and reduced self-esteem, etc. Because of all these reasons and more, all patients need to visit an oncologist for evaluation of the malignancy and relevant treatment if advised.
Another reason for testing abnormal skin lesions and bumps is the fact that the skin anomalies may be a symptom of some serious kind of skin cancer. This is especially true if the abnormal bumps fail to heal on its own over time; experience mild to profuse bleeding; tend to change in shape, size, and/or color; are sore, tender, or itchy; and/or are continuously exposed to the harsh rays of the sun.
Once the health care provider confirms a diagnosis of the abnormal bumps on skin as keratoacanthoma lesions, then he/she may recommend the below listed treatment options:
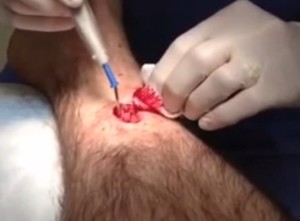
- Surgical excision of the keratoacanthoma bumps. The area is then sutured and bandaged.
- Radiation therapy and/or chemotherapy for eliminating the cancerous cells.
- Cryosurgery, wherein the abnormal skin lesions are frozen and destroyed through the use of liquid nitrogen
- Mohs micrographic surgical procedure, wherein the affected skin is surgically removed in layer till the entire keratoacanthoma is removed. This method is used to remove keratoacanthoma lesions from sensitive and tender regions like the nose, ears, lips, and hands.
Patients need to go for regular checkups to prevent a relapse of the skin cancer. It is also essential to follow the below listed precautionary measures to prevent new instances of keratoacanthoma lesions.
- The sun rays are its most intense between 10 AM and 3 PM. So avoid venturing outdoors during this time.
- Use a sunscreen with at least 30 SPF, along with other sun-protection items like sunglasses, hats, etc. when going outdoors.
- Do not stay in contact with UV light for long periods of time. This holds true for exposure to sunlight, artificial tanning machines, etc.