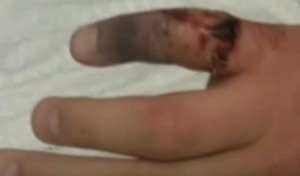
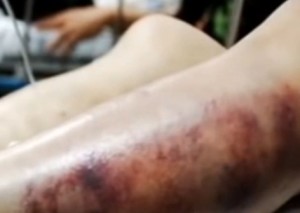
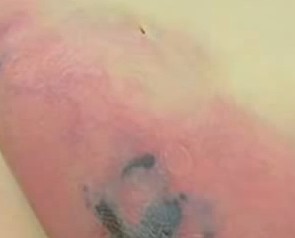
Necrotizing fasciitis or Flesh eating disease is one of the most severe bacterial infections that penetrates into a particular part of the human body and make the soft tissue of the body deteriorate. It looks as if the skin or the flesh has been eaten. In America almost 700 to 800 cases of the flesh eating disease are diagnosed every year. At least one fourth of the cases end up causing death. The disease isn’t usually diagnosed among children. Cases where the cause could not be known have often attracted medical attention.
Causes
This rare disease is a result of the bacteria, also known as type A bacteria or the group A strep. The signs and manifestation are not difficult to treat but the toxins released by the bacteria destroy the tissues eventually making it dead. They contaminate smooth layers of a membrane called fascia, which are connecting tissue bands that encompass blood vessels, fat, nerves and fat. Even the tissues close to the fascia can be affected.
The layer of the tissue that gets destroyed is the layer of connective tissue beneath the skin. It is highly recommended to have a timely and accurate diagnosis as well as effective and immediate treatment mostly done with the help of antibiotics or through a surgery. The bacteria can be contracted through an open cut, wound or a muscle strain. It is communicable and can be passed from person to person. Once the bacterium has entered into the body, it starts killing the tissue, skin and fat causing eventual organ failure or death. It works quickly leaving hardly any time for early treatment that includes antibiotics like penicillin and clindamycin. It is very important to fight the infection on time which means removing the infected area to stop further spread of the bacteria to other parts of the body.
Symptoms
The symptoms generally start showing up within a day of infection and include the following:
- Increase in the level of pain where there could be a small cut, abrasion or any other kind of skin opening. The level of pain could be more than what the cut or abrasion looks like.
- Redness, itching and heat like feeling around the affected area are common. Also there could be symptoms on other parts, especially the ones close to the affected area.
- Flu, diarrhea can also be experienced and one could feel nauseous and feverish accompanied by dizziness and weakness.
- One can also get dehydrated and feel excessively thirsty.
- In three to four days of the infection, there can possibly be swelling and a purple rash on and around the infected area.
- Violet colored rashes and marks that can turn into blisters filled with abscess that foul smells.
- Due to tissue death there’s peeling and flakiness of the skin.
- Severely low blood pressure and unconsciousness.
The symptoms can also be confusing appearing like some other illness. People suffering might at the same time complain of cramps, have a feeling of pulled muscle and soreness. There can be ulcers, blisters and spots that can vary in color and size. The confusing signs can also make the diagnosis more difficult and increase the complication. Therefore, having unusual symptoms after a wound or cut should not be taken casually and medical help should be taken at the earliest.
Is Necrotizing Fascitis contagious?
The flesh-eating disease is not contagious. The only way one can contract the disease is through expose to bacteria, like you would if you got a cut on your skin. .
Treatment
Usually the disease is treated with strong antibiotics injected into the vein. However the antibiotics cannot always affect the decaying and infected portions and the bacterial toxins can also harm the soft tissue and the blood flow. That is one reason why surgical intervention becomes so important to stop the infection.
In the case of antibiotics, the choice depends upon the type of bacteria as well and many doctors strongly recommend multiple antibiotics. In the case of a surgical intervention the choice has to be made depending upon the area that has been affected such as going for a urologic surgeon in case of Fournier’s gangrene. Most of the patients can be extremely sick and have to be admitted to an ICU. In some hospitals hyperbaric oxygen therapy is also given to promote tissue recovery. However this therapy alone cannot substitute antibiotics or surgical treatment.